What "This Activates Your Brain's Reward System" Actually Tells Us
“Activates your brain’s reward system” sounds precise. An examination of what that phrase actually measures—and why it rarely tells you what health claims imply.
Why neuroscience language travels so well
Open almost any wellness article, supplement description, or behavioral health explainer and the phrase appears reliably: this activates your brain's reward system. Sometimes it's dopamine. Sometimes it's the mesolimbic pathway. Sometimes it's just "your brain's pleasure centers." The framing shifts, but the implication stays the same—that science has identified something specific happening in the brain, and that this explains the behavior or outcome being described.
The phrase has become a staple of health communication because it works rhetorically. Neuroscience carries authority. A claim grounded in brain activity sounds more rigorous than one grounded in behavior or preference. It implies mechanism—not just that something happens, but why. And it suggests that the experience being described is real, measurable, and biologically significant.
All of this is true, up to a point. The reward system is a real neural circuit. Dopamine is a real neurotransmitter. But "activates your brain's reward system" has been applied to so many different phenomena, under such different conditions, that the phrase has largely stopped functioning as an explanation. Understanding what it actually describes—and what it doesn't—changes how much weight it should carry in decisions about products, behaviors, and health claims.
If you want a simple framework for evaluating new health studies in the news, subscribers receive a free guide: 5 Questions to Ask Before Believing a Health Headline
What the reward system actually is
The brain's reward system is a set of interconnected structures and pathways involved in motivation, learning, and the anticipation and experience of reward. The core circuit involves the ventral tegmental area, the nucleus accumbens, and the prefrontal cortex, connected by the mesolimbic dopamine pathway.
Dopamine, the neurotransmitter most associated with this system, plays a central role—but a more specific and more constrained one than popular accounts typically assign it. Rather than functioning as a simple pleasure signal, dopamine in the mesolimbic system is better understood as a learning and prediction signal. Dopamine neurons don't respond to reward in a straightforward way. They respond to deviations from learned predictions—what researchers call a prediction error signal. When an outcome is better than expected, dopamine activity increases. When it matches expectations, activity stays roughly flat. When it falls short, activity dips below baseline. As associations form over time, the signal transfers from the reward itself to the cues that reliably predict it.
This means dopamine is more closely tied to learning what to pursue and updating those predictions than to the raw experience of pleasure. The subjective feeling of enjoyment appears to rely more heavily on opioid and endocannabinoid signaling at specific "hedonic hotspot" regions, including the nucleus accumbens shell and the ventral pallidum. Dopamine stimulation in those same regions consistently fails to enhance hedonic reactions.
This distinction matters because much of what gets attributed to "reward system activation" in health content conflates several neurochemically distinct processes: the prediction signal that drives anticipation, the motivational drive to obtain a reward, the hedonic experience when it arrives, and the reinforcement that makes a behavior repeat. Collapsing all of that into a single phrase obscures what any specific claim is actually asserting.
What "activates" means—and doesn't mean
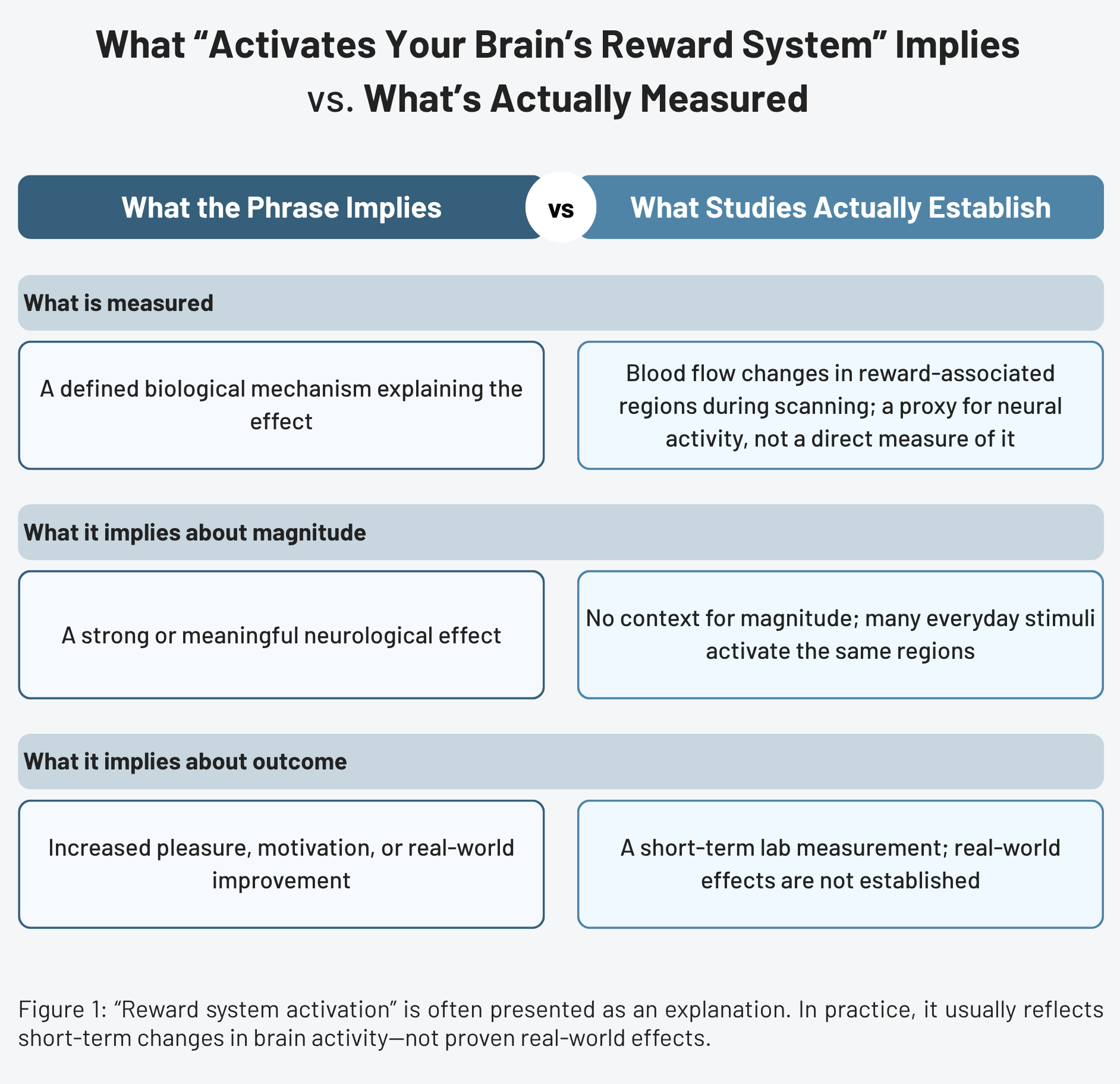
The language of "activation" is borrowed from neuroimaging research, particularly fMRI studies, which use changes in blood flow (the BOLD signal) as a proxy for neural activity. When a study reports that a food, supplement, or behavior "activates the reward system," it typically means that brain regions associated with reward processing showed measurable increases in activity during scanning.
In the right context, that’s a meaningful finding. Several limitations shape what it actually tells us, though.
For one, a very wide range of stimuli produce measurable activity in reward-associated brain regions—food, music, social connection, novelty, exercise, monetary gain, and many others. The reward system exists precisely to evaluate and respond to relevant stimuli in the environment. In many cases, saying something "activates the reward system" is roughly equivalent to saying the brain responded to something it found relevant. That observation doesn’t distinguish between stimuli in terms of magnitude, duration, clinical significance, or downstream consequence.
Magnitude matters—and it’s almost never communicated in health claims. A modest increase in nucleus accumbens activity in response to a supplement ingredient is a qualitatively different finding from the sustained, high-magnitude dysregulation associated with addictive substances. Both can be described as "activating the reward system," but they are not remotely equivalent in what they imply.
There's also a more fundamental issue: activation in a brain region during a task also doesn’t establish that the region caused the observed behavior, that the effect persists outside the scanner, or that it translates into any measurable real-world outcome. Neuroimaging research is fundamentally correlational—it identifies associations between neural activity and stimuli or experiences, but cannot on its own establish mechanisms or predict outcomes.
How the phrase gets used beyond its evidence
The gap between what neuroimaging findings actually show and how they appear in health and wellness content is substantial.
A common pattern: a study finds that a food ingredient, behavioral intervention, or supplement produces measurable activity in reward-associated brain regions in a small sample under controlled laboratory conditions. The finding is real. By the time it reaches product marketing or health content, it's often transformed into a general claim about what the product does to the brain—stripped of the qualifications that would make it accurate.
"Clinically proven to activate your brain's reward centers" may cite a real study. That study may have enrolled twenty participants, measured a surrogate marker of neural activity in a specific context, and reported a statistically significant but modest effect. The implication—that using the product reliably produces meaningful neurological changes that improve well-being—goes well beyond what the study demonstrated.
Dopamine in particular has become prone to this kind of overextension. The word now functions less as a scientific descriptor and more as a cultural shorthand for motivation, pleasure, and reward. Products promise to "boost dopamine," activities are described as "dopamine hits," and entire behavioral protocols are marketed around "dopamine optimization." Much of this language has drifted far enough from the underlying neuroscience that it carries little specific meaning.
The actual pharmacology of dopamine is considerably more complex. Dopamine acts through multiple receptor subtypes with distinct functions, operates across several neural pathways beyond the mesolimbic reward circuit–including pathways involved in movement, cognition, and neuroendocrine regulation–and its relationship to subjective experience is mediated by a range of individual, contextual, and neurobiological factors. Interventions claiming to "boost dopamine" are rarely evaluated against any of these specifics.
When reward system claims are grounded
Not all references to reward system activation are equally unsupported.
Research on addiction and substance use disorders has produced some of the most robust evidence linking reward system activity to behavioral and clinical outcomes. The mechanisms by which substances of abuse dysregulate dopamine signaling in the mesolimbic pathway are well characterized, replicated across many studies, and directly relevant to understanding dependence, tolerance, and treatment response. When addiction researchers and clinicians refer to reward system disruption, they are drawing on a substantive evidence base that connects specific mechanisms to specific outcomes in specific populations.
Research on the neurobiology of depression has similarly identified meaningful abnormalities in reward processing—reduced sensitivity to reward cues, altered dopamine function, and impaired motivation—that help explain clinical features like anhedonia and that have informed treatment development. These are specific, clinically grounded claims backed by decades of converging evidence across methodologies.
What separates these uses from the wellness marketing version isn’t that one invokes neuroscience and the other doesn't. The clinical and research applications specify mechanisms, populations, effect sizes, and outcomes. The marketing version extracts the language and leaves the substance behind.
Exercise sits somewhere in between. There is genuine evidence that regular aerobic exercise influences dopamine and serotonin signaling, and that these changes are associated with improvements in mood and cognitive function in certain populations. The evidence is more robust than most supplement claims—but also far more qualified than "exercise activates your reward system." The accurate version involves specifying what kinds of exercise, in what populations, with what effect sizes, over what time frame, and with the acknowledgment that the precise mechanisms are still being worked out.
How to read reward system claims more carefully
When you encounter a claim that something "activates the brain's reward system," a few questions can clarify what the evidence actually supports:
- What does the underlying study actually measure—brain imaging, behavioral outcomes, subjective experience, or something else?
- How large was the study, and how similar are the participants to the people the claim is aimed at?
- How does the magnitude of the observed effect compare to other stimuli that activate the same system?
- Is the claim about a momentary measurement in a controlled setting, or a sustained real-world outcome?
- What does the reward system activation supposedly explain or predict—and is that link established by the evidence, or assumed?
Why this matters
Neuroscience language does real work in health and wellness content. It lends authority to claims that would otherwise invite more scrutiny, implies a level of mechanistic understanding that may not exist, and shifts the conversation from "does this work?"—a question with a specific evidence standard—to "here is how it works"—a framing that presupposes the answer.
The reward system is genuinely important for understanding motivation, habit formation, addiction, and mental health, and the research on it has produced findings that have meaningfully advanced clinical practice. The issue is that health content invoking neuroscience consistently outpaces the evidence it’s citing.
"Activates your brain's reward system" is only informative when it specifies what was measured, in whom, to what degree, under what conditions, and how it connects to an outcome that matters. When it functions as a standalone explanation, the phrase tells us much less than it appears to.
Understanding that distinction doesn't make neuroscience less useful as a framework for thinking about behavior and health. It makes individual claims easier to evaluate on their merits, rather than on the authority of the vocabulary used to describe them.
References
- The Mysterious Motivational Functions of Mesolimbic Dopamine, Neuron
- Neurobiology of Reward-Related Learning, Neuroscience and Biobehavioral Reviews
- Dopamine, Prediction Error and Beyond, Neuroscientist
- The neuroscience of investing: fMRI of the reward system, Brain Research Bulletin
- Building a neuroscience of pleasure and well-being, Psychology of Well-Being
- Dopamine System Dysregulation in Major Depressive Disorders, International Journal of Neuropsychopharmacology
- Bidirectional Association between Physical Activity and Dopamine Across Adulthood—A Systematic Review, Brain Sciences

